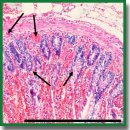
Trans-Serosal Multimodal Optical Coherence Tomography for Visualization of Microstructure and Blood Circulation of the Small Intestine Wall
The aim of the study was to evaluate the performance of trans-serosal multimodal OCT (MM OCT) in in vivo detecting of changes in microstructure and blood circulation of the small intestine wall caused by arteriovenous ischemia resulted from intestine strangulation.
Materials and Methods. In experiments on Wistar rats (n=22), we examined the small intestine wall in vivo using MM OCT; the access to the intestine was reached through laparotomy. The microvasculature and microstructure of the wall were studied before and after acute arteriovenous ischemia created by ligation of a small bowel segment. The results were then added with data obtained from histological and intravital microscopic examination.
Results. Trans-serous MM OCT allowed us to visualize the bowel wall to its entire thickness, distinguish between the serous-muscular and mucous-submucosal layers, and detect the villi and functioning blood vessels. The structures were best seen after a fat emulsion had been administered into the bowel lumen. In OCT images made in the optical coherent angiography (OCA) mode, large paired vessels (arteries and veins) and micro-vessels with a diameter of >15 μm could be seen. Most of the blood vessels were imaged in the depth range of 80–300 μm from the surface. Capillaries with a diameter of 7–10 μm were not seen, but they produced an overall bright background. In the OCA images reconstructed from a volume of 2.4×2.4×1.8 mm, the total length of the vascular bed before ischemia was 18.3 [16.6; 19.8] mm.
Strangulation of the intestinal loop was associated with changes in the CP OCT picture: the villi-associated vertical pattern and shadows of blood vessels disappeared and the depth of tissue visualization in the cross- channel decreased. The optical equivalents of the serous-muscular layer were preserved; after 180±12 min of ischemia, their proportion in the intestinal wall thickness increased from 25 [18; 32] to 42 [31; 55]% (p=0.031). At that time-point, OCA images of the strangulated bowel loop looked all similar: a uniform dark background with isolated fragmentary large vessels and no signs of blood flow in the microvascular network.
Conclusion. Trans-serous MM OCT provides for in vivo visualization of microstructures critical for surgical gastroenterology: the intestinal wall layers including villi and blood vessels of each layer, as confirmed by histological analysis. Destructive processes in the intestinal wall resulting from bowel ligation bring about optical changes, which can be detected using real-time MM OCT.
- Urbanavičius L., Pattyn P., de Putte D.V., Venskutonis D. How to assess intestinal viability during surgery. World J Gastrointest Surg 2011; 3(5): 59–69, https://doi.org/10.4240/wjgs.v3.i5.59.
- Bryski M.G., Frenzel Sulyok L.G., Kaplan L., Singhal S., Keating J.J. Techniques for intraoperative evaluation of bowel viability in mesenteric ischemia: a review. Am J Surg 2020; in press, https://doi.org/10.1016/j.amjsurg.2020.01.042.
- Tsai T.H., Leggett C.L., Trindade A.J., Sethi A., Swager A.F., Joshi V., Bergman J.J., Mashimo H., Nishioka N.S., Namati E. Optical coherence tomography in gastroenterology: a review and future outlook. J Biomed Opt 2017; 22(12): 1–17, https://doi.org/10.1117/1.JBO.22.12.121716.
- Liot E., Assalino M., Buchs N.C., Schiltz B., Douissard J., Morel P., Ris F. Does near-infrared (NIR) fluorescence angiography modify operative strategy during emergency procedures? Surg Endosc 2018; 32(10): 4351–4356, https://doi.org/10.1007/s00464-018-6226-9.
- Lim C., Malek A., Martins R., Petillon S., Boulate G., Hentati H., De’Angelis N., Brunetti F., Salloum C., Laurent A., Compagnon P., Azoulay D. Real-time assessment of intestinal viability using indocyanine green fluorescent imaging (with video). J Visc Surg 2015; 152(1): 71–72, https://doi.org/10.1016/j.jviscsurg.2014.09.008.
- Alander J.T., Kaartinen I., Laakso A., Pätilä T., Spillmann T., Tuchin V.V., Venermo M., Välisuo P. A review of indocyanine green fluorescent imaging in surgery. Int J Biomed Imag 2012; 2012(7): 1–26, https://doi.org/10.1155/2012/940585.
- Reginelli A., Iacobellis F., Berritto D., Gagliardi G., Di Grezia G., Rossi M., Fonio P., Grassi R. Mesenteric ischemia: the importance of differential diagnosis for the surgeon. BMC Surg 2013; 13(Suppl 2): S51, https://doi.org/10.1186/1471-2482-13-S2-S51.
- Tateishi S., Arima S., Futami K. Assessment of blood flow in the small intestine by laser Doppler flowmetry: comparison of healthy small intestine and small intestine in Crohn’s disease. J Gastroenterol 1997; 32(4): 457–463, https://doi.org/10.1007/BF02934083.
- Bajory Z., Szabó A., Deák G., Varga R., Pajor L. Orthogonal polarization spectral imaging: a novel tool for examination of microcirculatory changes in the testis. J Androl 2012; 33(3): 499–504, https://doi.org/10.2164/jandrol.111.013599.
- de Bruin A.F., Kornmann V.N., van der Sloot K., van Vugt J.L., Gosselink M.P., Smits A., Van Ramshorst B., Boerma E.C., Noordzij P.G., Boerma D., van Iterson M. Sidestream dark field imaging of the serosal microcirculation during gastrointestinal surgery. Colorectal Dis 2016; 18(3): O103–O110, https://doi.org/10.1111/codi.13250.
- Drexler W., Liu M., Kumar A., Kamali T., Unterhuber A., Leitgeb R.A. Optical coherence tomography today: speed, contrast, and multimodality. J Biomed Opt 2014; 19(7): 071412, https://doi.org/10.1117/1.JBO.19.7.071412.
- Leitgeb R.A., Baumann B. Multimodal optical medical imaging concepts based on optical coherence tomography. Front Phys 2018; 6(114), https://doi.org/10.3389/fphy.2018.00114.
- Jäckle S., Gladkova N., Feldchtein F., Terentieva A., Brand B., Gelikonov G., Gelikonov V., Sergeev A., Fritscher-Ravens A., Freund J., Seitz U., Schröder S., Soehendra N. In vivo endoscopic optical coherence tomography of esophagitis, Barrett’s esophagus, and adenocarcinoma of the esophagus. Endoscopy 2000; 32(10): 750–755, https://doi.org/10.1055/s-2000-7711.
- Zuccaro G., Gladkova N., Vargo J., Feldchtein F., Zagaynova E., Conwell D., Falk G.W., Goldblum J., Dumot J., Ponsky J., Gelikonov G., Davros B., Donchenko E., Richter J. Optical coherence tomography of the esophagus and proximal stomach in health and disease. Am J Gastroenterol 2001; 96(9): 2633–2639, https://doi.org/10.1111/j.1572-0241.2001.04119.x.
- Tsai T.H., Lee H.C., Ahsen O.O., Liang K., Giacomelli M.G., Potsaid B.M., Tao Y.K., Jayaraman V., Figueiredo M., Huang Q., Cable A.E., Fujimoto J., Mashimo H. Ultrahigh speed endoscopic optical coherence tomography for gastroenterology. Biomed Opt Express 2014; 5(12): 4387–4404, https://doi.org/10.1364/BOE.5.004387.
- Samel N.S., Mashimo H. Application of OCT in the gastrointestinal tract. Appl Sci 2019; 9(15): 2991, https://doi.org/10.3390/app9152991.
- Gelikonov V.M., Romashov V.N., Shabanov D.V., Ksenofontov S.Yu., Terpelov D.A., Shilyagin P.A., Gelikonov G.V., Vitkin I.A. Cross-polarization optical coherence tomography with active maintenance of the circular polarization of a sounding wave in a common path system. Radiophys Quant El 2018; 60(11): 897–911, https://doi.org/10.1007/s11141-018-9856-9.
- Moiseev A., Ksenofontov S., Gorozhantseva M., Shakhova N., Sirotkina M., Kiseleva E., Matveev L., Zaytsev V., Zagaynova E., Gelikonov V., Gladkova N., Vitkin A., Gelikonov G. Real time OCT-based angiography device with hand-held probe for everyday clinical use. J Biophotonics 2018; 11: e201700292, https://doi.org/10.1002/jbio.201700292.
- Roggan A., Doerschel K., Minet O., Wolff D., Müller G. The optical properties of biological tissue in the near infrared wavelength range: review and measurements. In: Laser-induced interstitial thermotherapy. Bellingham: SPIE Press; 1995; p. 10–44.
- Maslennikova A.V., Sirotkina M.A., Moiseev A.A., Finagina E.S., Ksenofontov S.Y., Gelikonov G.V., Matveev L.A., Kiseleva E.B., Zaitsev V.Y., Zagaynova E.V., Feldchtein F.I., Gladkova N.D., Vitkin A. In-vivo longitudinal imaging of microvascular changes in irradiated oral mucosa of radiotherapy cancer patients using optical coherence tomography. Sci Rep 2017; 7(1): 16505, https://doi.org/10.1038/s41598-017-16823-2.
- Kawada K., Hasegawa S., Wada T., Takahashi R., Hisamori S., Hida K., Sakai Y. Evaluation of intestinal perfusion by ICG fluorescence imaging in laparoscopic colorectal surgery with DST anastomosis. Surg Endosc 2017; 31(3): 1061–1069, https://doi.org/10.1007/s00464-016-5064-x.
- Stacey R., Green J.T. Radiation-induced small bowel disease: latest developments and clinical guidance. Ther Adv Chronic Dis 2014; 5(1): 15–29, https://doi.org/10.1177/2040622313510730.
- Gordeeva A.E., Sharapov M.G., Tikhonova I.V., Chemeris N.K., Fesenko E.E., Novoselov V.I., Temnov A.A. Vascular pathology of ischemia/reperfusion injury of rat small intestine. Cells Tissues Organs 2017; 203(6): 353–364, https://doi.org/10.1159/000455830.
- Sergeev A.M., Gelikonov V.M., Gelikonov G.V., Feldchtein F.I., Kuranov R.V., Gladkova N.D., Shakhova N.M., Snopova L.B., Shakhov A.V., Kuznetzova I.A., Denisenko A., Pochinko V.V., Chumakov Yu.P., Streltzova O.S. In vivo endoscopic OCT imaging of precancer and cancer states of human mucosa. Opt Express 1997; 1(13): 432–440, https://doi.org/10.1364/oe.1.000432.
- Pfau P.R., Sivak M.V. Jr., Chak A., Kinnard M., Wong R.C., Isenberg G.A., Izatt J.A., Rollins A., Westphal V. Criteria for the diagnosis of dysplasia by endoscopic optical coherence tomography. Gastrointest Endosc 2003; 58(2): 196–202, https://doi.org/10.1067/mge.2003.344.
- Gora M.J., Suter M.J., Tearney G.J., Li X. Endoscopic optical coherence tomography: technologies and clinical applications [Invited]. Biomed Opt Express 2017; 8(5): 2405–2444, https://doi.org/10.1364/BOE.8.002405.
- Masci E., Mangiavillano B., Albarello L., Mariani A., Doglioni C., Testoni P.A. Pilot study on the correlation of optical coherence tomography with histology in celiac disease and normal subjects. J Gastroenterol Hepatol 2007; 22(12): 2256–2260, https://doi.org/10.1111/j.1440-1746.2006.04725.x.
- Masci E., Mangiavillano B., Barera G., Parma B., Albarello L., Mariani A., Doglioni C., Testoni P.A. Optical coherence tomography in pediatric patients: a feasible technique for diagnosing celiac disease in children with villous atrophy. Digest Liver Dis 2009; 41(9): 639–643, https://doi.org/10.1016/j.dld.2009.02.002.
- Lee H.-C., Fass O., Ahsen O.O., Liang K., Wang Z., Figueiredo M., Potsaid B., Jayaraman V., Huang Q., Fujimoto J.G., Mashimo H. Endoscopic optical coherence tomography microangiography identifies the altered microvasculature of the terminal ileum in Crohn’s disease. Gastrointest Endosc 2017; 85(5): AB511–AB512, https://doi.org/10.1016/j.gie.2017.03.1180.










